Psychotic symptoms in children and adolescence, such as paranoia, hallucinations, and delusions, are relatively common and can be associated with a range of diagnoses. Nevertheless, their presence understandably leads to tremendous concern on the part of patients, families, and clinicians about the possibility of an emerging thought disorder such as schizophrenia. This article offers important long-term data regarding the outcome of early appearing psychotic symptoms.
Study participants come from the well-known Dunedin Multidisciplinary Health and Development Study, which is perhaps best known for a landmark gene-environment interaction study. The sample included 1037 individuals who were evaluated initially at the age of 11 for psychotic symptoms using a structured interview and followed until age 38.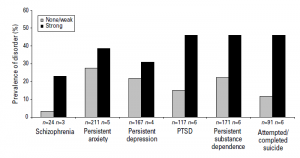
A total of 1.7% of children at age 11 reported clear psychotic symptoms. By age 38, 3.7% of the sample had been diagnosed with schizophrenia or met criteria for the illness. Results showed that psychotic symptoms present at age 11 were significantly associated with schizophrenia. A total of 23% of those with psychotic symptoms at age 11 had the diagnoses as compared to 3% of those without clear childhood symptoms, for a relative risk of 7.24. However, children with psychotic symptoms were also at significantly elevated risk for PTSD (RR=3.03) and suicide attempts (RR=3.82). The rate of adult PTSD in the group with child psychotic symptoms was 46.2%, and few were free of any diagnosable psychopathology. None of those children with psychotic symptoms at age 11 went on to be diagnosed with an episode of mania.
The authors concluded that early appearing psychotic symptoms was a risk factor for later schizophrenia but was also related to adult PTSD and suicide attempts. Overall, child psychotic symptoms appeared to be a strong indicator for higher levels of adult psychopathology in general.
While the overall n of the study is impressive, it is important to remember that the n for most of these analyses was only 13. Nonetheless, the conversion rate to schizophrenia of 23% among those with early psychotic symptoms is similar to other reports and is a percentage that clinicians might want to remember when talking to families. The lack of bipolar disorder is also worth mentioning as conventional wisdom from much of the American literature suggests a strong link between psychotic symptoms in childhood and bipolar disorder.
Reference
Fisher et al. (2013). Specificity of childhood psychotic symptoms for predicting schizophrenia by 38 years of age: A birth cohort study. Psychol Med, January, 1-10
Tags: psychosis, schizophrenia

