This post was written by Gregory Paylor ’18
In the US, health insurance coverage was broadened and expanded under The Affordable Care Act. While this reduced the total uninsured population, cost per unit of care went unaddressed and the model of healthcare delivery has remained largely unchanged. Only recently have we begun to see payment model initiatives attempting to address healthcare payment reform and improvement to patient outcomes. Because of this, insurers have been looking for other ways to reduce downstream healthcare spending. This is where the Social Determinants of Health (SDOH) come into play.
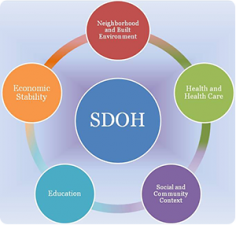 The World Health Organization (WHO) defines SDOH as “the conditions in which people are born, grow, live, work and age. These circumstances are shaped by the distribution of money, power and resources at global, national and local levels. The social determinants of health are mostly responsible for health inequities – the unfair and avoidable differences in health status seen within and between countries.” Examples of SDOH include: safe housing, food availability, segregation, exposure to crime, presence of trash, transportation options, and the natural environment.
The World Health Organization (WHO) defines SDOH as “the conditions in which people are born, grow, live, work and age. These circumstances are shaped by the distribution of money, power and resources at global, national and local levels. The social determinants of health are mostly responsible for health inequities – the unfair and avoidable differences in health status seen within and between countries.” Examples of SDOH include: safe housing, food availability, segregation, exposure to crime, presence of trash, transportation options, and the natural environment.
Massachusetts, New York, Oregon, Utah, and Vermont are all “testing strategies not only to link Medicaid and social services, but also to use Medicaid funds to actually deliver supportive services that affect social determinants of health. These value-based delivery system reforms include the creation of accountable care organizations, health homes, community health teams, and accountable communities for health.”
Rather than waiting for patients to come into the ER or be seen when a problem manifests, developing a network of community partners to proactively engage healthcare consumers is a preventative strategy that is important to take note of. Insurers are making a point to positively influence the social conditions of its members as a way to save money on medical bills that could potentially occur. This type of upfront investment has the potential to bring down healthcare spending while improving the health of underserved and vulnerable patient populations.
